The Critical Importance of Healthcare Facility Cleaning
Healthcare facility cleaning is a specialized process that protects patients, staff, and visitors from harmful pathogens and infections.
Key Elements:
- Purpose: Prevents healthcare-associated infections (HAIs)
- Frequency: General areas daily; high-risk areas 2+ times daily
- Standards: Follows CDC, OSHA, EPA guidelines
- Methods: Uses specific cleaning patterns (cleaner-to-dirtier, high-to-low)
- Equipment: Employs hospital-grade disinfectants, microfiber cloths, HEPA vacuums
- Staff: Requires specialized training on infection control
According to the CDC, healthcare-associated infections affect about 1 in 31 hospital patients on any given day in the United States. This statistic underscores why proper cleaning protocols are essential for patient safety.
Unlike standard commercial cleaning, healthcare cleaning demands rigorous adherence to specific protocols, comprehensive training, and specialized products. It's the difference between a space that looks clean and one that is truly sanitized.
Healthcare facilities represent environments where inadequate cleaning can be life-threatening. Operating rooms, patient rooms, emergency departments, and waiting areas all require different approaches to minimize infection risk.
I'm RJ Patel, founder of PCT Janitorial, with over four decades of experience in healthcare facility cleaning protocols that exceed industry standards while ensuring regulatory compliance and patient safety.
What Is Healthcare Facility Cleaning?
Healthcare facility cleaning is far more than just mopping floors and wiping surfaces. It's a carefully orchestrated process designed to create safe spaces for healing by breaking the chain of infection.
Unlike cleaning at home or in an office building, medical cleaning faces unique challenges:
- Dealing with potential bloodborne pathogens and infectious materials
- Meeting dramatically higher standards because lives depend on proper disinfection
- Adapting approaches for different areas (waiting rooms vs. operating theaters)
Environmental cleaning in healthcare settings focuses on two main types of surfaces:
- High-touch surfaces – Items everyone touches: doorknobs, light switches, bed rails, call buttons, and IV poles. These need frequent attention.
- Low-touch surfaces – Areas with minimal contact like floors, ceilings, and walls still need regular cleaning, just not as frequently.
The consequences of inadequate cleaning are sobering – approximately 1 in 31 hospital patients will develop a healthcare-associated infection on any given day in the United States.
Staff who perform healthcare facility cleaning need specialized training that includes OSHA Bloodborne Pathogens Standards, proper PPE use, chemical handling, and infection control principles.
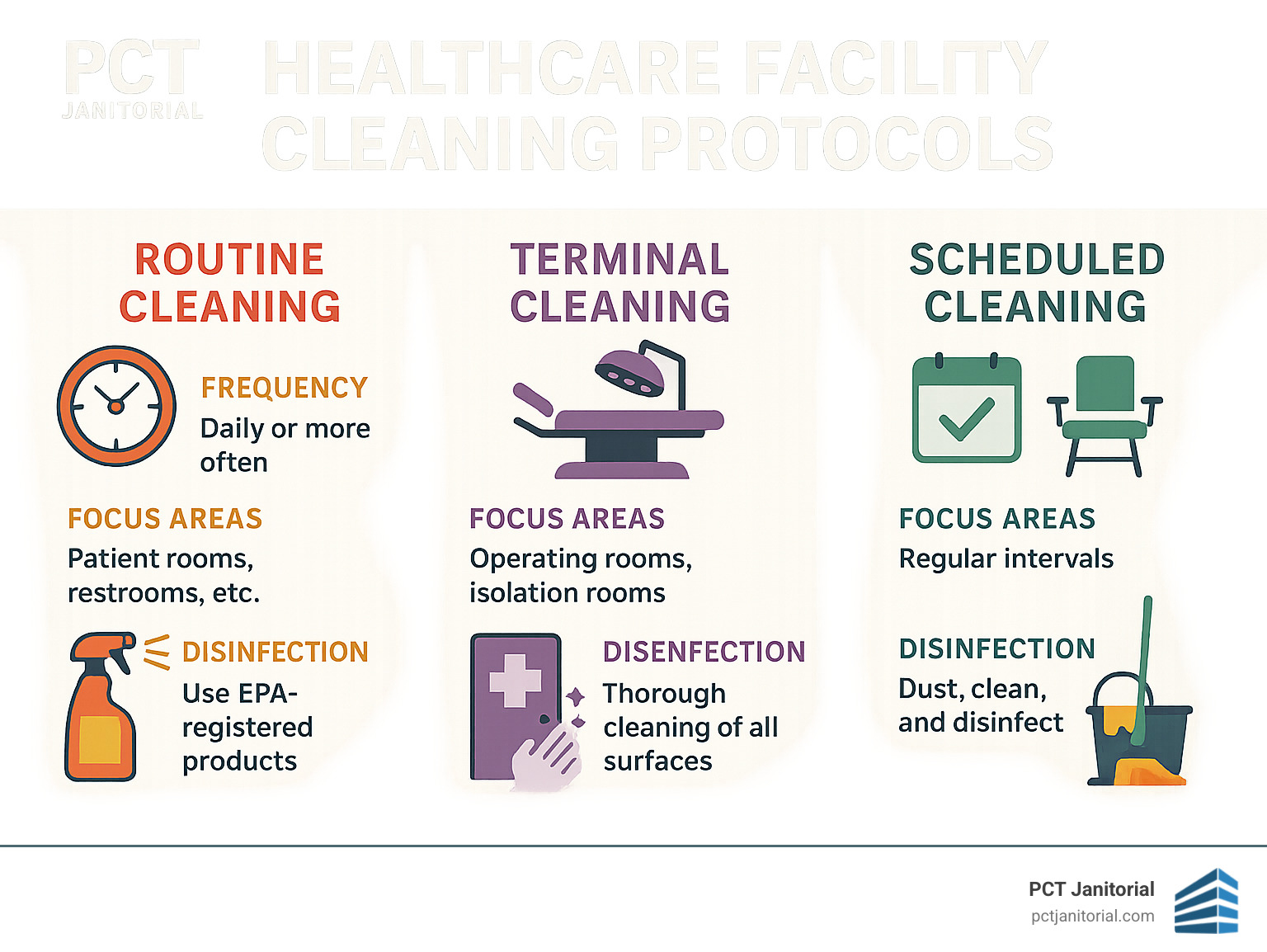
Routine Healthcare Facility Cleaning vs Terminal Cleaning
Healthcare facility cleaning includes different approaches for different situations:
| Cleaning Type | Definition | Frequency | Focus Areas |
|---|---|---|---|
| Routine Cleaning | Daily cleaning while patient is present | At least once every 24 hours | High-touch surfaces, visible soil, bathrooms |
| Terminal Cleaning | Thorough cleaning after patient discharge | After each discharge or transfer | All surfaces, equipment, curtains, mattresses |
| Scheduled Cleaning | Periodic deep cleaning | Weekly, monthly, or quarterly | Floors, walls, ceilings, vents, light fixtures |
Routine cleaning is daily maintenance focusing on high-touch surfaces and visible soiling. Terminal cleaning is the comprehensive approach that happens after a patient leaves. Scheduled cleaning tackles areas that don't need daily attention but still matter for overall environmental hygiene.
High-Risk Areas Requiring Specialized Healthcare Facility Cleaning
Some departments need extra special attention:
Operating Rooms (ORs)
These spaces require terminal cleaning between each procedure with special attention to surgical lights, tables, and equipment.
Intensive Care Units (ICUs)

ICUs house the most vulnerable patients with compromised immune systems. High-touch surfaces need cleaning at least twice daily, with special attention to ventilator equipment and monitoring devices.
Isolation Wards
These areas require pathogen-specific cleaning protocols depending on what's being isolated. Cleaning staff need appropriate PPE and dedicated cleaning equipment.
Emergency Departments (EDs)
With high patient turnover, there's a need for frequent spot cleaning. Cleaning staff need to balance thoroughness with quick turnaround times.
Regulations & Industry Standards You Must Follow
When it comes to healthcare facility cleaning, following regulations isn't just a good idea—it's necessary. These standards exist to protect everyone in your facility.
The CDC offers evidence-based recommendations that evolve as we learn more about infection control. They provide guidance on cleaning frequency based on risk and specific protocols for handling various pathogens.
OSHA focuses on keeping cleaning staff safe through their Bloodborne Pathogens Standard, requiring proper exposure control plans, appropriate PPE, and comprehensive training.
The EPA handles disinfectants, with their List N identifying products effective against specific pathogens. They set standards for how these products should be used, from contact times to application methods.
CMS ties Medicare and Medicaid reimbursements directly to infection prevention measures, while The Joint Commission evaluates environmental cleaning during accreditation.
According to scientific research on infection-control standards, facilities that follow these guidelines see dramatic reductions in infection rates.
For Georgia healthcare facilities, there's an additional layer of state-specific regulations from the Georgia Department of Public Health.
OSHA Bloodborne Pathogens & HazCom Essentials
The OSHA Bloodborne Pathogens Standard (29 CFR 1910.1030) protects cleaning staff from potentially infectious materials.
Personal protective equipment includes appropriate gloves for all cleaning tasks, face shields when splashing might occur, fluid-resistant gowns in potentially contaminated areas, and proper respiratory protection for airborne precaution rooms.
Sharps management requires puncture-resistant containers for disposal and protocols for handling dropped sharps safely.
Every facility needs a written exposure control plan that's updated annually and accessible to all employees.
Staff training must happen when someone is hired, with refreshers at least annually, and any time procedures change.
The Hazard Communication Standard (HazCom) requires Safety Data Sheets for all cleaning chemicals, proper labeling of containers, and employee training on chemical hazards.
At PCT Janitorial, our Preventative Care services include comprehensive assistance with BBP and HazCom compliance.
CDC/EPA Disinfection Requirements
All disinfectants used in healthcare must be EPA-registered and appropriate for specific needs:
- List N products are effective against COVID-19
- Hospital disinfectants tackle common healthcare pathogens
- Tuberculocidal disinfectants for tougher challenges
- Sporicidal disinfectants for C. difficile spores
Contact time is how long a surface needs to stay wet with disinfectant to kill germs. Different products have different requirements, typically ranging from 1-10 minutes.
Concentration matters tremendously. Using the wrong dilution won't work and might create resistant germs.
How you apply these products is just as important as which ones you choose. Use enough product to thoroughly wet surfaces, apply with friction, and never dry-wipe before the contact time is complete.
Special situations require special approaches. C. difficile needs sporicidal products, norovirus requires products with specific norovirus claims, and bloodborne pathogens need intermediate-level disinfection.
The CDC emphasizes: "cleaning must precede disinfection." Organic material can neutralize disinfectants, making them ineffective.
Area-By-Area Cleaning Procedures & Best Practices
Effective healthcare facility cleaning requires a systematic approach. Our teams start with a quick visual assessment to spot visible soil and potential hazards before planning their cleaning sequence.
We follow key principles:
- Cleaner-to-dirtier: Starting with the cleanest areas before progressing to more contaminated spaces
- High-to-low: Beginning with liftd surfaces before moving to mid-level counters and finishing with floors
- Consistent directional pattern: Working clockwise or counterclockwise to ensure nothing is missed

Color-coding prevents cross-contamination: red tools for high-risk areas like isolation rooms and bathrooms, yellow for patient rooms, green for food service areas, and blue for lower-risk spaces.
Microfiber cloths and mops trap and remove 99% of bacteria (compared to just 30% with traditional cotton), while HEPA vacuums capture 99.97% of particles 0.3 microns or larger.
We've replaced traditional mop buckets with no-dip flat mop systems that eliminate cross-contamination from dirty mop water.
Exam & Waiting Rooms
In waiting areas, check-in counters and reception desks need special attention, with high-touch surfaces disinfected hourly during busy periods. Seating requires daily cleaning of chair arms and backs, while children's play areas need careful management of toys and activities.
For exam rooms, we follow a two-tiered approach:
- Between patients (5-7 minutes): Disinfecting the exam table, cleaning equipment used during examination, wiping down high-touch surfaces
- End of day (15-20 minutes): More thorough cleaning of all surfaces, restocking supplies, mopping floors, emptying waste receptacles
Our Disinfecting Cleaning services pay special attention to frequently overlooked areas like magazine racks, water fountains, and HVAC vents.
Operating Rooms & ICUs
Operating rooms follow a rigorous cleaning sequence between cases (20-30 minutes) and more intensive terminal cleaning (60-90 minutes) after the last case of the day.
ICUs require high-touch surfaces to be cleaned at least twice daily, with dedicated cleaning tools that remain in the unit. Ventilators, monitoring equipment, and bed areas all need specialized attention.
Restrooms & Spills of Blood/Body Fluids
Restrooms in healthcare settings need cleaning at least three times daily, working from cleaner to dirtier areas—starting with mirrors and counters before moving to sinks and dispensers, and finishing with toilets and floors.
For blood and body fluid spills, we follow a specific two-step process:
- Containment: Donning appropriate PPE, containing the spill with absorbent materials, and placing biohazard warning signs
- Cleaning and disinfection: Removing visible material, cleaning with detergent, and disinfecting with an appropriate intermediate-level disinfectant
Noncritical Equipment & High-Touch Surface List
Noncritical equipment includes items that contact intact skin but not mucous membranes, such as blood pressure cuffs, thermometers, mobility devices, and monitoring equipment.
High-touch surfaces with the highest contamination rates include bed rails (93%), IV poles (87%), call buttons (82%), overbed tables (80%), and doorknobs (76%).
In general care areas, high-touch surfaces need attention every 4 hours, while in high-risk areas like ICUs, that frequency doubles to every 2 hours.
Products, Equipment & Protective Gear
The right tools are essential for effective healthcare facility cleaning. Hospital-grade disinfectants must be EPA-registered with appropriate healthcare claims, including EPA List N products effective against COVID-19.
Quaternary ammonium compounds tackle a wide range of bacteria and viruses, while improved hydrogen peroxide formulations offer broader protection with less waiting time. For C. difficile spores, bleach solutions at the right concentration are often necessary.
Specialized equipment includes microfiber technology that traps 99% of bacteria and HEPA filtration vacuums that capture nearly all particles 0.3 microns or larger. Some facilities employ no-touch disinfection systems using UV-C light or hydrogen peroxide vapor.
Personal protective equipment (PPE) selection is based on the specific cleaning task and risk level:
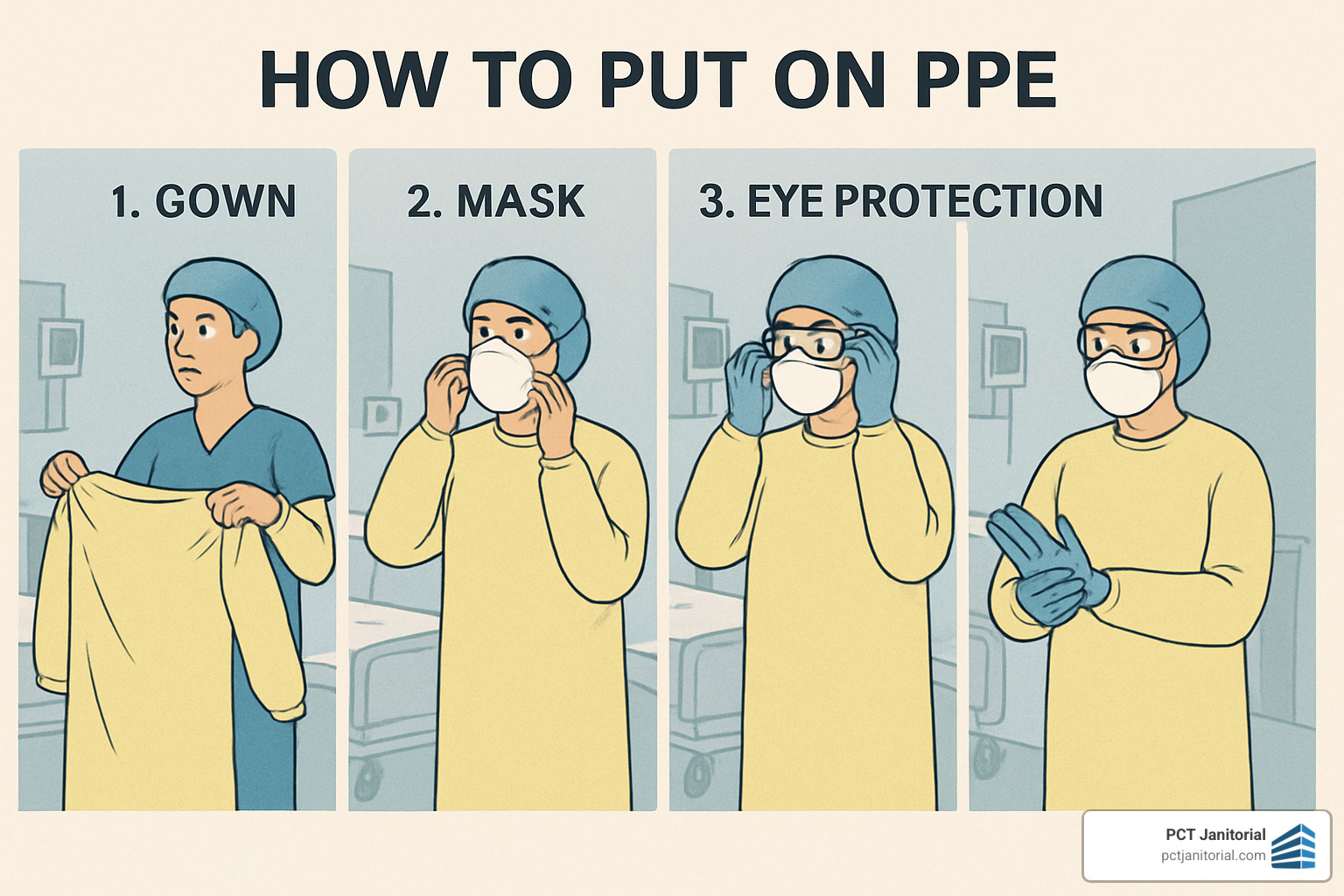
- Standard precautions: Task-appropriate gloves, clean uniform, and closed-toe shoes
- Moderate risk: Fluid-resistant gowns, face masks, and eye protection
- High-risk areas: Task-specific gloves, impervious gowns, N95 respirators for airborne precautions
The sequence of putting on (donning) and removing (doffing) PPE is critical to prevent contamination.
Selecting the Right Disinfectant
Choosing the right disinfectant requires considering several factors:
- Efficacy: What pathogens does it kill?
- Contact time: How long must surfaces stay wet? (1-5 minutes is ideal)
- Material compatibility: Will it damage surfaces?
- Safety: What are the toxicity and irritation risks?
- Ease of use: Ready-to-use vs. concentrates
Quaternary ammonium compounds work well for general surface disinfection but have limitations against certain viruses. Improved hydrogen peroxide formulations offer excellent broad-spectrum coverage with good material compatibility. Bleach remains effective against C. difficile and norovirus but is corrosive to metals.
All disinfectants must be used exactly according to label instructions—using a product differently than directed isn't just ineffective, it's against federal law.
Managing Supplies & Waste Safely
Effective inventory control maintains par levels for all cleaning supplies, uses the first-in, first-out (FIFO) method, and includes monthly audits to prevent shortages.
Chemical storage requires secure, well-ventilated areas with secondary containment for liquid concentrates. All containers must be clearly labeled, and incompatible chemicals kept separate.
Healthcare facilities generate multiple waste streams requiring specific handling:
- Regulated medical waste: Blood-soaked items and materials contaminated with potentially infectious body fluids
- Sharps waste: Needles, scalpels, and broken glass in puncture-resistant containers
- Pharmaceutical waste: Categories for hazardous and non-hazardous medications
- General waste: Office materials, food packaging, and non-contaminated items
Most facilities implement a color-coded waste system: red for biohazardous waste, yellow for chemotherapy waste, black/clear for general waste, blue for recycling, and white for pharmaceutical waste.
Our Protection & Disinfection services include comprehensive waste management protocols to ensure compliance with all applicable regulations.
Monitoring, Training & Compliance Assurance
Effective healthcare facility cleaning requires robust quality assurance systems. Our multi-layered approach to monitoring includes:
- Direct observation of cleaning procedures
- Visual inspections using standardized checklists
- Fluorescent marking systems applied to high-touch surfaces before cleaning
- ATP bioluminescence testing to detect organic residue that might harbor pathogens
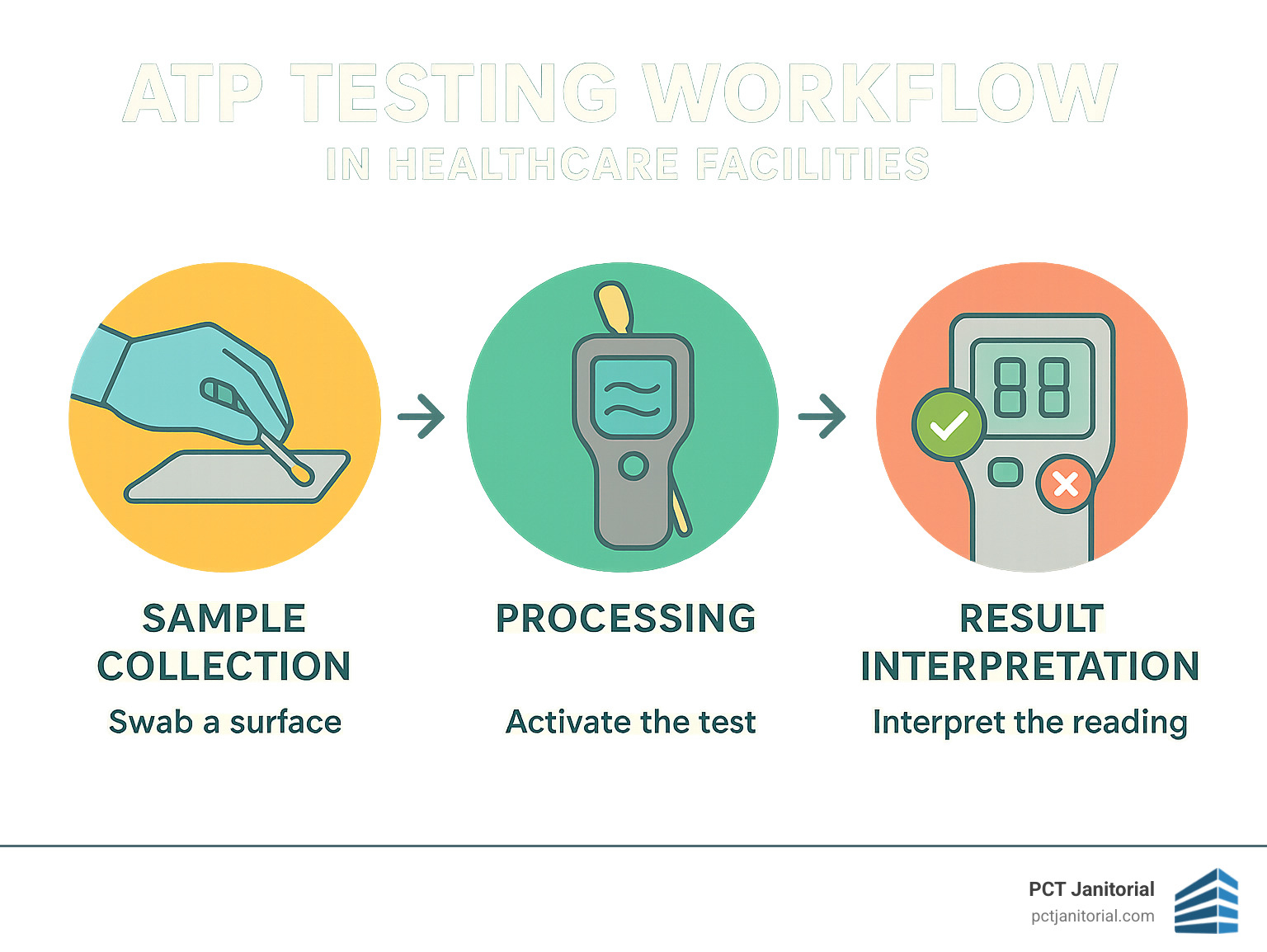
Comprehensive documentation includes cleaning schedules, completed checklists, training certifications, monitoring results, product usage logs, equipment maintenance, and incident reports.
Our continuous improvement cycle follows a simple pattern: establish baseline performance, implement targeted interventions, measure results, standardize successful changes, and identify the next opportunity for improvement.
Research shows facilities with comprehensive monitoring programs have demonstrated up to 80% reduction in surface contamination and significant decreases in healthcare-associated infections.
Building an Audit Program
An effective audit program combines daily quick checks with deeper periodic assessments. We use random selection to prevent predictability and ensure all department types are evaluated.
Our performance metrics establish realistic improvement targets based on baseline data, with department-specific standards based on risk level.
When issues are identified, our corrective action process kicks in immediately. Critical findings are addressed on the spot, while systemic issues undergo root cause analysis.
Our scoring system includes:
- Score 5 (Excellent): Exceeds standards
- Score 4 (Good): Meets all standards
- Score 3 (Acceptable): Minor deficiencies
- Score 2 (Below Standard): Notable deficiencies
- Score 1 (Unacceptable): Major deficiencies
The most successful audit programs engage stakeholders at all levels and focus on improvement rather than punishment.
Staff Education & PPE Drills
Our training approach begins with comprehensive new employee orientation covering infection prevention principles, chemical safety, bloodborne pathogen protocols, proper cleaning sequences, and documentation requirements.
Annual refresher training ensures everyone stays current with evolving best practices and regulatory requirements. Competency assessments include hands-on skills demonstration to ensure staff can perform critical tasks correctly.
PPE drills ensure staff can properly protect themselves during cleaning tasks, particularly in high-risk situations. Each drill presents a realistic scenario where staff must demonstrate they can select appropriate PPE, don it correctly, maintain proper technique during cleaning, and safely remove contaminated items.
Our Healthcare Facility Cleaning Service emphasizes these educational components because facilities with robust training programs consistently demonstrate higher protocol compliance and lower infection rates.
Frequently Asked Questions about Healthcare Facility Cleaning
How often should different hospital areas be cleaned?
Cleaning frequencies vary based on risk level:
High-risk areas like operating rooms need cleaning between each procedure, with terminal cleaning at day's end. ICUs, isolation rooms, and emergency departments need high-touch surfaces disinfected every 2-4 hours.
Medium-risk areas like patient rooms need full cleaning daily and terminal cleaning after each patient leaves. Treatment rooms need cleaning between each patient use.
Lower-risk areas like waiting rooms need high-touch surfaces cleaned 2-3 times daily and full cleaning once a day. Administrative areas need daily cleaning.
Beyond daily routines, we also tackle monthly wall cleaning, quarterly ceiling maintenance, and regular attention to light fixtures and HVAC vents.
Which PPE is mandatory for cleaning staff?
PPE requirements depend on the cleaning environment:
For standard areas, basics include gloves, clean uniforms, and closed-toe shoes.
In moderate-risk areas where splashing might occur, we add fluid-resistant gowns, surgical masks, and eye protection.
High-risk areas require more comprehensive protection. For rooms with contact precautions, staff wears gloves and isolation gowns. For droplet precautions, we add face shields. For airborne precautions, our teams use N95 respirators or PAPRs.
Blood spill response requires heavy-duty gloves, impervious gowns, and face shields.
PCT Janitorial provides all necessary PPE at no cost to our employees, ensures proper fit, maintains adequate supplies, and provides thorough training.
What is the difference between detergent and disinfectant?
Detergents contain surfactants that break down dirt, grime, and organic material so it can be wiped away. They physically remove germs rather than killing them. Common examples include neutral floor cleaners and enzymatic cleaners.
Disinfectants are chemical agents that damage or destroy pathogens on surfaces. While detergents might remove 90-99% of germs through physical cleaning, disinfectants kill 99.9-99.9999% of what remains. These products are regulated by the EPA with specific claims about what germs they kill.
Many disinfectants don't work well in the presence of dirt and organic material. That's why we typically use a two-step process:
- Clean with a detergent to remove visible soil and reduce the number of germs
- Apply a disinfectant to kill the remaining pathogens
As the CDC emphasizes, "cleaning must precede disinfection" because organic material can shield germs from disinfectants.
Conclusion
Effective healthcare facility cleaning is a critical component of patient safety, infection prevention, and regulatory compliance. The specialized techniques we've discussed—moving from cleaner areas to dirtier ones, and working from high surfaces down to low—minimize cross-contamination and protect vulnerable patients.
Hospital-grade disinfectants with specific contact times are your first line of defense against pathogens. The difference between routine daily cleaning, terminal cleaning, and scheduled deep cleaning addresses different levels of risk at appropriate intervals.
Regulatory compliance isn't optional in healthcare environments. The documentation and monitoring systems we've outlined provide proof that you're doing everything possible to protect patients and staff.
Advanced cleaning technologies make a significant difference. Microfiber systems capturing 99% of bacteria means the difference between a surface that looks clean and one that truly is clean. HEPA filtration prevents harmful particles from being redistributed into the air. Quality monitoring tools like ATP testing verify cleaning effectiveness.
Staff training and PPE protocols form the foundation everything else builds upon. When your team understands not just what to do but why they're doing it, compliance improves dramatically.
Studies consistently show that improved environmental cleaning can reduce healthcare-associated infections by up to 80% in some settings. This translates to shorter hospital stays, reduced healthcare costs, improved patient outcomes, and saved lives.
At PCT Janitorial, our specialized teams serving Kennesaw, Acworth, Atlanta, Marietta, and throughout North Georgia are thoroughly trained in healthcare-specific cleaning protocols. We offer a free, comprehensive hygiene assessment using scientific testing methods to help healthcare facilities identify improvement opportunities and ensure compliance with all relevant standards.
For more information about our Healthcare Facilities cleaning services, contact us today. Your patients deserve nothing less than the highest standards of environmental hygiene.


